Local Tempe Teeth Whitening Clinic: Safe and Effective Options
If you’re searching for a local Tempe teeth whitening clinic, Tempe Family Dentistry is the ideal place to achieve a brighter, healthier smile. Our experienced dental team offers
Cosmetic Dentist Tempe: Veneers vs. Other Cosmetic Dentistry Options
A bright, beautiful smile can make a world of difference in your confidence and overall appearance. With the rise in cosmetic dentistry options in Tempe, AZ, more people are explor
Snap-In Dentures: The Future of Comfort and Stability
In recent years, denture technology has advanced by leaps and bounds, bringing innovative solutions to those seeking comfortable, functional, and aesthetically pleasing dental opti
Understanding Cosmetic Dentistry: Best Cosmetic Dentist Near Me
When it comes to enhancing your smile, finding the best cosmetic dentist near you is important. A perfect smile not only boosts your confidence but also plays a significant role in
Dental Cleaning: Essential for Your Oral Health
Maintaining good oral health is not just about having a bright smile; it’s about taking care of your overall well-being. At Tempe Family Dentistry, we understand the vital ro
Affordable Dentures and Implants: Signs You Might Need Them
Maintaining good dental health is necessary for your overall well-being. At Tempe Family Dentistry, we understand that sometimes, despite our best efforts, circumstances can lead t
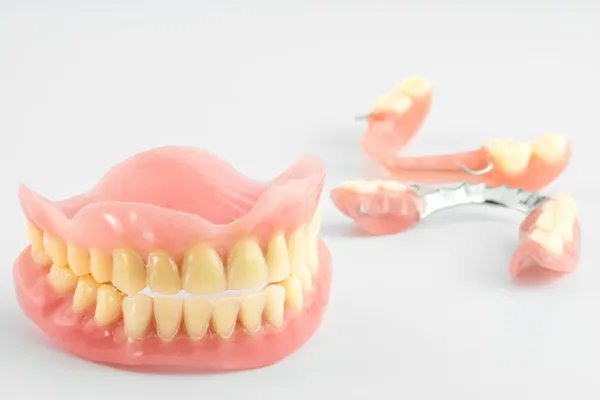
What Are Partial Dentures?
Partial dentures are removable dental appliances used to replace one or more missing teeth. Unlike full dentures, which replace all teeth in an arch, partial dentures fit around ex
Denture Implants or Traditional Dentures? How to Choose the Right Dentures
Dentures play an important role in restoring dental health and enhancing quality of life for many individuals. Whether you’re missing a few teeth or need full-mouth restorati
The Complete Guide to Dentures: Everything You Need to Know Including Dentures Cost
Dentures are essential dental prosthetics that restore functionality and aesthetics for individuals experiencing tooth loss. Understanding the various types of dentures and associa
Sonic Denture Cleaners: A Hygienic Innovation for Your Dentures
Maintaining the cleanliness of your dentures is essential for your oral health. Traditional cleaning methods, while effective to some extent, often fall short in removing all the p